Introduction
Sacrospinous ligament fixation (SSLF) is a surgical technique used for the treatment of a type of pelvic organ prolapse, which involves the roof (apex) of the vagina. In such an apical prolapse, the uterus (womb) can herniate, and this is called a uterine prolapse. In patients with previous hysterectomy, the top of the vagina can also prolapse (vault prolapse).
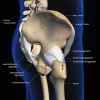
In the human pelvis, there are ligaments, which are strong bands of connective tissue that connect bones together. One such example is the sacrospinous ligament, which connects the ischial spine (a bony notch in the lower pelvis) to the sacrum (bottom of the spine). There is a sacrospinous ligament on each left and right side. Sutures can be placed on this ligament and then attached to the apex of the vagina or cervix. When tied down, this will reduce the apical prolapse to an inside, supported position. These sutures can be either permanent or slowly absorbed over time. They are replaced by strong scar tissue eventually.
Sometimes the iliococcygeus (a pelvic floor muscle) muscle can be used to place these sutures instead of the sacrospinous ligament. This is called an iliococcygeus suspension.
Indications
SSLF is used to treat women with apical prolapse (uterus, vault, enterocele). It can preserve the vaginal length.
SSLF can be done in women who still wish to preserve their uterus, or together with a vaginal hysterectomy in those who don’t. In some patients, it is done together with other vaginal prolapse repairs, or during incontinence surgery.
It is a comparatively less invasive option to a transabdominal sacrocolpopexy, and has very good success rates (80% - 90%).
Preoperative Instructions
If you are taking blood thinners or certain newer diabetic medications, please inform your doctor as these may have to be stopped before the surgery.
You will need to fast for at least 6 hours before the surgery.
Your doctor may require you to have blood tests or a urine test prior to the surgery.
See preparing for surgery, for more detailed instructions.
Procedure
The surgery can be done under general or spinal anaesthetic. Intravenous antibiotics are given. A catheter is placed to drain the bladder.
A posterior compartment vaginal incision is done. An anterior approach can also be done in patients who need a concurrent cystocele repair. The vagina is freed up from the underlying fascia and rectum. Further dissection is done to allow access to the sacrospinous ligament, which is identified using bony landmarks and palpation. 1 to 2 sutures are placed through the ligament and secured to the vaginal apex. This can be done on one side or both (left and right) sides.
Other vaginal prolapse repair is done if necessary, and the vaginal skin is closed. A pack is placed in the vagina.
Postoperative Instructions
Most patients stay in the hospital for 1 to 2 days. The vaginal pack is removed on day 1. Patients are encouraged to mobilise. The catheter is removed on either day 1 or 2, depending on your pain level and mobility. If the patient is voiding satisfactorily, she can then go home.
About 1 in 6 patients may get deep-seated buttock pain. This is due to the suture that is placed in the deep pelvic ligament. This pain can be felt on one side only, or on both sides. Occasionally if it is severe, the patient is kept in the hospital for a few more days for pain relief. It is expected to slowly resolve but a few weeks to a few months. It is very rare to get chronic pain from this. An anti-inflammatory pain relief suppository is usually very effective for this.
The vaginal incision usually does not cause much post-op pain. Some creamy white vaginal discharge may be expected for the first few weeks. This is due to the presence of dissolvable sutures in the vagina. About a week post-op, some blood-stained vaginal discharge may happen. This is due to the breakdown of old blood trapped under the skin. If the discharge is offensive-smelling, see your GP in case you need to go on oral antibiotics.
You can do light duties at home including walking up 1-2 flights of stairs, going for short walks, and going to the shops (but no heavy lifting) in the first few weeks. Slowly increase your activity level as you become more comfortable.
Take your pain medication as directed. You may need to take it as soon as you start feeling uncomfortable (before the pain gets severe).
Do not drive for at least 2 weeks as you may still have some post-op pain.
No sexual intercourse for 6 weeks as the vaginal wound needs time to heal.
Check with your doctor when you can go back to work as the type of work that you do will determine this. In general, if your work is not too physically demanding, you can go back to work in 3 to 4 weeks. If it is more demanding, you may need about 6 weeks off work.
You should attend your post-op appointment so your doctor can check for any complications.
Risks
General risks:
- Anaesthetic risks such as heart or lung problems.
- Wound infection – you will be covered with antibiotics during the surgery.
- Bleeding – it is uncommon (<1%) to need a blood transfusion for this surgery.
- Clots in the legs (DVT) or pulmonary emboli.
- Chest infection, urinary tract infection.
- Allergic reactions (e.g., to dressings, drugs etc.) – inform us if you have any known allergies.
- Risk of death is a very rare complication that may arise from any surgery or anaesthetic. Modern medicine and anaesthesia have made this extremely rare. The risk varies with each individual’s general health conditions and the complexity of the surgery. The sacrospinous ligament fixation surgery is not considered to be a major surgery.
Specific risks:
- Buttock pain as described above. Most of these settle down within 6 weeks.
- Damage to surrounding organs such as the rectum, ureters, or bladder. This is very rare and is usually identified and repaired during the surgery.
- Painful intercourse (5%) after surgery. Some women find intercourse less uncomfortable after the prolapse is repaired.
- Constipation. Drink lots of water and have a high-fibre diet to treat this.
Treatment Alternatives
See pelvic organ prolapse, for further discussion about other treatment alternatives.